Thyroid Eye Disease
What is Thyroid Eye Disease?
Thyroid Eye Disease (TED) is an autoimmune condition most commonly linked with Grave’s Disease (hyperthyroidism). However, it can be linked with other thyroid conditions like Hashimoto’s Disease and thyroid cancer. In some cases, patients may have no thyroid abnormality at all at diagnosis (euthyroid thyroid eye disease).
Table of Contents
ToggleIn TED, the white blood cells in the body produce antibodies that react with the thyroid gland and the tissues around the eye (orbit). This can cause bulging of the eyes, swollen eyelids, difficulty moving the eyes, double vision, dry eyes, lashes rubbing on the surface of the eye, and a change in appearance of the eyes and face.
At a more microscopic level, these changes may be occurring:- The fat behind the eye enlarges, pushing the eye outward
- The muscles that move the eye become tight and scarred, causing double vision
- The muscles that move the eye become enlarged and swollen. In the worst cases, this can compress the optic nerve and cause vision loss.
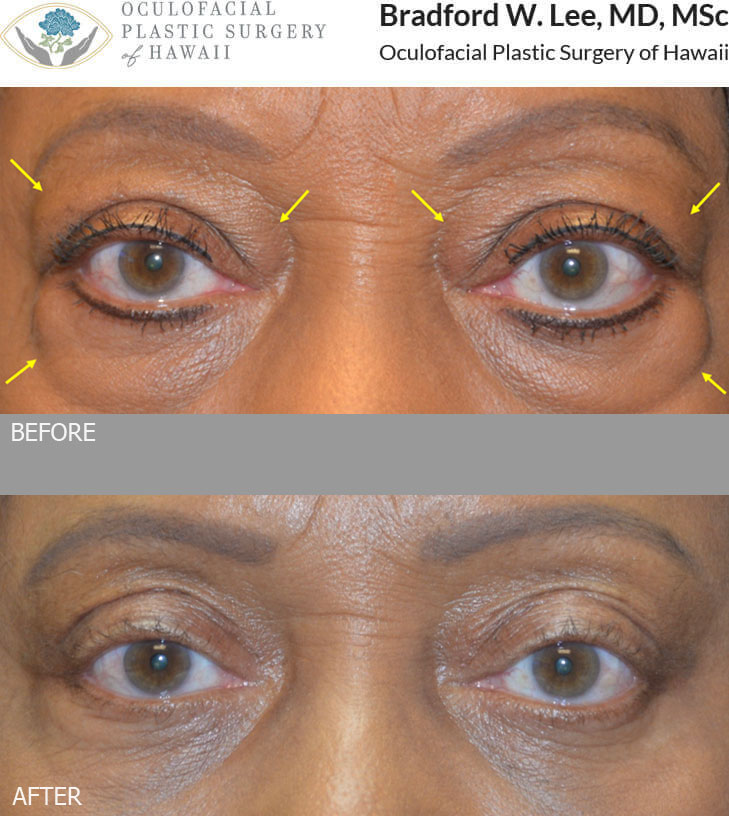
This 67-year-old lady had a history of thyroid eye disease and was bothered by prominent excess fat and skin on the upper and lower eyelids. She underwent a bilateral upper and lower blepharoplasty with orbital fat decompression that subtly improved the bulging of the eyes, softened her expression, and rejuvenated the upper and lower eyelids.
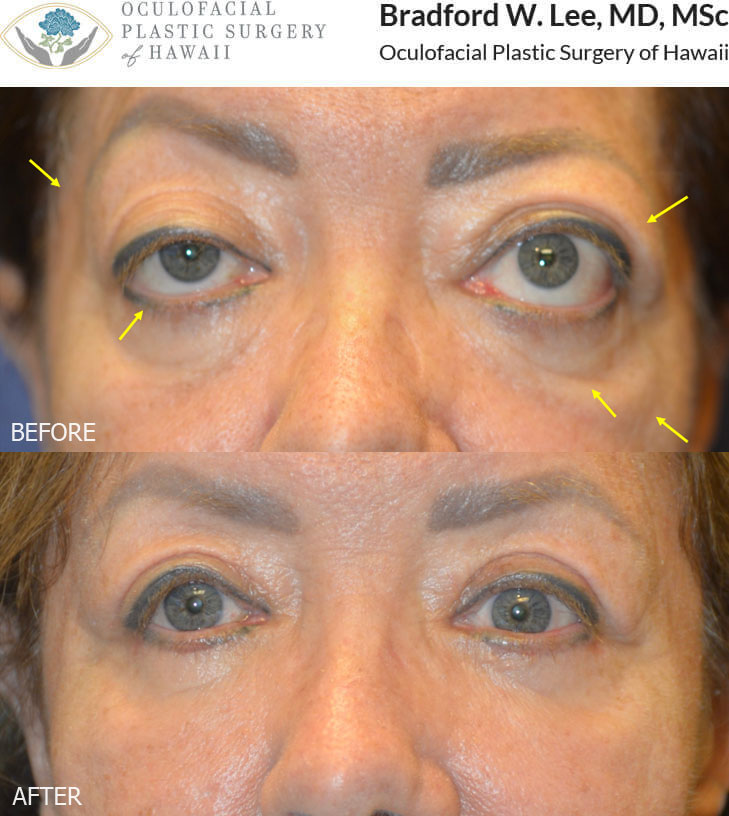
This 60+ year-old lady with thyroid eye disease was bothered by the bulging of her eyes, lower eyelid retraction, excess skin on both upper and lower eyelids, and age-related atrophy of the temples, under eye region, and cheeks. She underwent bilateral orbital decompression surgery, eyelid retraction repair, quad blepharoplasty, and fat transfer to the temples, cheeks, and lower lids to reduce the bulging of the eyes, improve the position and symmetry of the eyelids, and restore youthful facial contours in the periocular region.
What can make TED better or worse?
Things that make TED better or help prevent its development include:
- Maintaining normal thyroid hormone levels
- Selenium supplements, 200 mcg daily (helpful especially if deficient in Selenium)
- Statin cholesterol medications (reduces development and severity)
- Thyroidectomy (helpful when thyroid levels are hard to control)
Things that make TED more likely and more severe:
- Poorly controlled thyroid levels
- Tobacco smoke
- Radioactive iodine (especially if no steroids are given with it)
Finally, a blood test called Thyroid Stimulating Antibody (TSI) is closely associated with disease activity and progression in TED and can be monitored periodically along with thyroid levels.
What are the traditional treatments for Thyroid Eye Disease?
TED has an “active” inflammatory phase early on but eventually progresses to a “quiescent” phase that has fewer inflammatory signs. All medical therapies are aimed to treat “active inflammation” and are less effective in the later, quiescent stage of disease.
Traditional therapies used to treat TED include:
- Oral steroids: pills that are taken daily to suppress TED inflammation
- Steroid infusions: weekly intravenous infusions work like oral steroids but are more effective with less side effects
- Steroid injections around the eye: performed by an ophthalmologist to help reduce swelling of the eyelid and cheek and can correct upper eyelid retraction early in disease.
- Radiation therapy: low-dose radiation is administered in 10 short sessions over 2 weeks to help with double vision, difficulty moving the eye, and compression of the optic nerve
What are the newer treatments for TED?
Some of the newer and most effective treatments for TED are “biologicals,” or antibody therapies that selectively target parts of the inflammatory process. They are often prescribed by a rheumatologist and may be indicated for other autoimmune conditions. They require periodic lab tests to monitor safety. Because these medications can be very expensive, insurance companies have a strict authorization process for their use in TED.
The most promising biologicals include:- Teprotumumab (Tepezza): the only FDA-approved treatment for TED. It is given as an intravenous infusion ever 3 weeks over 6 months and reduces inflammation and bulging of the eyes while helping double vision and quality of life.
- Tocilizumab (Actemra): this medication is available as a monthly IV infusion or as a convenient self-administered subcutaneous injection given every 1-2 weeks. It is used off-label for TED but has been well studied and is effective in controlling challenging cases of TED, even where steroids or radiation have failed.
- Rituximab (Rituxan): this medication is an IV infusion that targets the B cells (white blood cells) responsible for causing inflammation in TED. It is an immunosuppressive medication that is used off-label for TED and given in two doses early in the inflammatory phase.

Testimonials




How does rehabilitative surgery work for TED?
The focus of treatment during the active, inflammatory phase of disease is on controlling inflammation with the treatments listed above. Once the inflammation resolves and the disease becomes quiescent, the focus shifts toward rehabilitative surgery to help patients restore their eyes and appearance.
The rehabilitative process is broken up into 3 stages, although many patients are able to skip one or more of the stages:
- Orbital decompression surgery: to address bulging of the eyes
- Strabismus surgery: to address double vision and correct the alignment of the eyes
- Eyelid surgery: to address any eyelid retraction, drooping, or excess skin or fat
Orbital decompression surgery is typically done in an ambulatory surgery setting (Dr. Lee does this at Queen’s Medical Center Same Day Surgery) under general anesthesia. Although it is possible to do both sides at the same time, many patients choose to have one side done first and the second side done 1-2 weeks later to make recovery easier. Each side can take anywhere from 1-2.5 hours depending on how large a decompression is need to address the bulging.
Strabismus surgery is done by a strabismus specialist, and Dr. Lee will work with you on partnering with one of his colleagues who focus on correcting double vision. Strabismus surgery is done at an outpatient surgery center and can be performed starting 3 months after orbital decompression. If patients have only mild double vision, they may not require surgery and could use prisms in their glasses instead.
Eyelid surgery again may not be necessary in some cases, or can be combined with the orbital decompression surgery. It normally consists of raising or lowering the eyelid to the proper position (e.g. eyelid retraction repair, ptosis repair) or removing excess skin and fat (e.g. upper blepharoplasty, lower blepharoplasty). Eyelid surgery can be performed with local anesthesia in the office or with IV sedation in an outpatient surgery center. Surgery can take 1-2 hours, depending on what procedures are being done. Patients go home the same day and are able to have their eyes open immediately after surgery.
How does Dr. Lee Customize rehabilitative surgery for TED?
Orbital decompression surgery is one of the most challenging surgeries performed by oculofacial plastic surgeons, and to do them well requires extensive experience and advanced training. TED surgery was one of the focuses of Dr. Lee’s academic practice at Bascom Palmer Eye Institute, and he has performed over 200 orbital decompressions over his career and lecture extensively on this surgery around the world.
Orbital decompression surgery must be performed so that the eye goes back into the eye socket by a precise amount, ranging from about 2-10 mm. Different walls of the eye socket can be expanded, and a quantity of fat behind the eye can also be removed. In select cases, Dr. Lee uses intraoperative navigation technology to more precisely remove bone and achieve the best surgical outcomes.
Eyelid and facial surgery are again highly customized and more challenging in TED. Every patient needs something slightly different to restore the appearance of their eyes and face. As an expert in cosmetic and reconstructive eyelid and facial surgery, Dr. Lee will work with you to help restore your “pre-disease appearance” and can also offer additional procedures to treat the signs of aging if desired.
Does insurance cover rehabilitative surgery for TED?
Insurance typically covers most of the rehabilitative procedures for TED, such as orbital decompression, strabismus surgery, eyelid retraction repair, or ptosis repair. It typically does not cover upper blepharoplasty or lower blepharoplasty.
What is the “down time” after Entropion Repair?
Orbital decompression surgery typically results in some bruising and swelling of the eyelid which improves quickly over the first few weeks after surgery. Patients have their “final result” about 3 months after surgery. Patients are given a pain medications, a short course of oral steroids, antibiotic ointment, and sometimes an oral antibiotic as well.After eyelid surgery, patients should expect some bruising and swelling for at least 1-2 weeks. Most patients look good by 1 month after surgery when most of the swelling is gone. The “final result” is at 2-3 months after surgery.
After either of these surgeries, patients apply ice to the eyelids for the first 2-3 days after surgery to reduce the swelling. There is minimal pain after surgery, and most patients simply use ice and Tylenol for any discomfort. Vision may be slightly blurry for a few days due to eyelid swelling and the antibiotic ointment. Patients can walk around the same day of surgery and do light activities, including using the computer or watching TV. They should avoid heavy lifting, straining, or bending for the first 2 weeks. Patients who have had orbital decompression are asked not to blow their nose or pinch their nose when they sneeze for the first two months after surgery. Antibiotic ointment is applied to the incisions for the first two weeks.
Schedule Your Consultation Today
TED is a challenging disease that can cause discomfort, affect vision, and transform facial appearance, and affect numerous psychological and social aspects of patients lives. Dr. Lee enjoys treating this challenging condition and is specially trained to help TED patients control the inflammatory process and restore the appearance and function of their eyes. Schedule your consultation today to learn more and take the first steps toward overcoming TED.


